AIDS
AIDS (acquired immunodeficiency syndrome) is defined as the stage of infection with HIV-1, or HIV (human immunodeficiency virus), in which an infected person's immune system has become so weak that he or she is at risk of developing other infections or cancers (or has already developed them) that can potentially lead to death. Though all people with AIDS are infected with HIV-1, not all people with HIV-1 infection have AIDS, nor will all of them develop AIDS.
HIV Pathogenesis
The cause of AIDS is human immunodeficiency virus-1 (HIV-1), a member of a group of viruses called retroviruses. Retroviruses are enveloped ribonucleic acid (RNA) viruses that contain an enzyme (reverse transcriptase) that will transcribe viral RNA to deoxyribonucleic acid (DNA). In the case of HIV-1, this DNA (now called a DNA provirus) is then integrated into the infected person's DNA. When the infected person's DNA is then transcribed, or read by the cell's molecular machinery, the proviral DNA is also read, leading to the creation of new virus and release from the infected cell.
The pathogenesis of HIV-1 infection is complex. HIV-1 binds to cells that have specific types of molecular receptors on their surface, such as CD4 and chemokine receptors. Cells that have these receptors include CD4 lymphocytes, macrophages, and microglial cells in the brain. CD4 lymphocytes are a kind of helper T cell . Macrophages are immune cells that consume infected cells, and microglial cells perform certain immune functions in the brain. After the virus binds and enters the cell, it will replicate as discussed above. In the course of a day, as many as ten billion virus particles can be produced in an infected person.
CD4 lymphocytes are one of the main targets of HIV-1. These cells are essential in the functioning of the immune system. The CD4 lymphocytes are destroyed by direct viral killing, by other lymphocytes that destroy HIV-infected cells, and probably by other mechanisms. As the CD4 lymphocytes
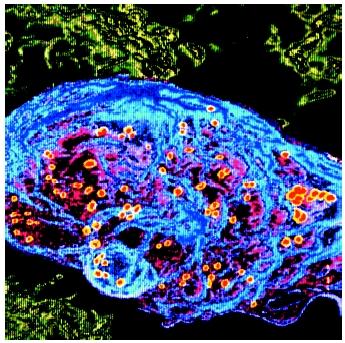
Transmission
The epidemiology of HIV infection/AIDS has changed over the years. When the disease was first recognized in the early 1980s, men who had sex with men were by far the largest affected risk group, followed by intravenous drug users who were sharing needles, individuals who received HIV-infected blood, and hemophiliacs who received infected clotting factors. Women who had sexual contact with infected men were recognized as being at high risk of contracting HIV, and if they were pregnant, passing it on to their unborn children.
Though this disease was first recognized in the United States, cases soon appeared in many countries of the world. Particularly hard hit were countries in sub-Saharan Africa, the Caribbean, and Asia. At the turn of the twenty-first century, it is estimated that more than forty million people are infected worldwide and as many as one million in the United States alone.
Transmission of HIV-1 occurs through infected bodily fluids. Sexual contact by far is the most common mode of transmitting HIV. Anal sex is the most efficient sexual manner of transmitting the virus. Vaginal intercourse poses the next highest risk, but more to the female than the male. In other words, it is much easier for an infected man to infect a woman through penile-vaginal intercourse than the other way around, especially if the man is circumcised and has no sores or ulcers on his penis. Since HIV is a blood-borne infection, those individuals engaging in intravenous drug use and sharing needles can easily transmit the virus in this manner. Prior to testing for the virus in the blood supply, there was a risk of acquiring HIV from transfusion of blood or a blood product, but this risk is now extremely small. Vertical transmission, or transmission from mother to child during pregnancy, occurs in about one-third of HIV-infected pregnant women who are not treated with anti-HIV medications.
Prevention
Prevention of HIV transmission is both a behavioral and medical problem. Abstinence from sexual behavior is promoted as the only sure way of preventing transmission of HIV. Though this of course is true, premarital and extramarital sexual behavior is common in most societies. Condoms provide an effective barrier to sexual transmission. Social, religious, political, and cultural issues, however, enter into the education of youth on the use of condoms, and lead to controversies over education about sexual behavior in general. With as many as one-third or more of HIV infections occurring during adolescence, aggressive and honest educational approaches must be implemented. One can only make an informed decision about one's behavior if one understands the consequences and has knowledge of how to prevent transmission.
Beyond all of this, there are the medical areas of transmission prevention. As mentioned above, HIV-infected pregnant women who are treated with anti-HIV medications can reduce their risk of transmitting the virus to their baby. Health care workers who are stuck with needles contaminated with blood from HIV-positive patients can reduce their risk of infection by using anti-HIV medications. Medical studies in the early twenty-first century are looking at the possibility of reducing the risk of HIV transmission following a sexual contact by treating the uninfected contact with anti-HIV medications. Vaccines against HIV are being researched in many parts of the world, but as of yet, have not been shown to be protective.
Treatment
Treatment of HIV/AIDS is both complicated and expensive. The medications that are available inhibit the reverse transcriptase enzyme, and inhibit an enzyme that helps the virus mature into one that can infect other cells. By using a combination of at least three different medications that are active at these various sites, one can clear the blood stream completely of virus. Once this occurs, the patient's immune system often improves, and in some cases, returns to normal. If the patient takes medications as directed and the virus stays suppressed, there is a chance that the patient may never become ill. The virus, however, is still present in the lymph nodes and probably other tissues. If the patient stops taking medications or takes them erratically, the virus will return to the bloodstream. Once the virus is actively produced again, there is a high probability that it will mutate to a form resistant to the medications that the patient was previously on. When this occurs, especially if the patient has been on more than one regimen of medicines, a virus resistant to all available medications can be selected for. At this point, little else can be done. One major concern about these individuals is that if they are still sexually active or continue to share needles, they will transmit resistant virus. This is being documented more frequently.
New medications are being studied that may be able to overcome this resistance problem by attacking different sites of viral production, or those that are not affected by mutations in the resistant virus. The problems here include the possibility that the patient could die before the new medicines are available; that if the patient is still alive, he or she will be unable to tolerate the side effects of the new medicines; and, finally, that the patient will be unable to afford the medicines. Anti-HIV or anti-retroviral medications are very expensive, costing over $10,000 per year in the United States. This, plus the costs of blood tests and doctor visits, makes treatment beyond the means of most of the infected people in the world.
HIV/AIDS is and will continue to be one of the greatest medical challenges medical professionals have ever faced. Prevention and education are the only means that public health professionals currently have to stem the tide of this ever-growing epidemic .
SEE ALSO Birth Control ; Retrovirus ; Reverse Transcriptase ; Sexually Transmitted Diseases ; T Cells ; Viral Diseases
Harold P. Katner
Bibliography
"Defeating AIDS: What Will It Take?" Scientific American 279, no. 1 (July 1998): 81–107.
Jasny, Barbara, ed. "AIDS: The Unanswered Questions." Science (special AIDS issue), 260 (28 May 1993): 1253–1293.
Mandell, G. L., J. E. Bennett, and R. Dolin, eds. Principles and Practice of Infectious Diseases, 5th ed. Philadelphia, PA: Churchill Livingstone, 2000.
Sande, M. A., and P. A. Volberding, eds. The Medical Management of AIDS, 6th ed. Philadelphia, PA: W. B. Saunders, Co., 1999.
World Health Organization. "WHO Global AIDS Statistics." AIDS Care 2000 12, no. 798.
Comment about this article, ask questions, or add new information about this topic: