Reproductive Technology
Reproductive technologies are medical procedures designed to help infertile people have children. These procedures include artificial insemination, in vitro fertilization , embryo adoption, and surrogate mothers.
Artificial Insemination
In artificial insemination (AI), sperm are collected from a man and placed into the female's uterus by a reproductive specialist. AI is often used for men with low sperm counts, men with genetic disorders, and women who wish to become pregnant without a male partner. Sperm used in AI may come from a known donor or an anonymous sperm bank.
In Vitro Fertilization
The first "test tube" baby, Louise Brown, was born in England in 1978. Since then, hundreds of thousands of babies have been born using in vitro fertilization and related techniques. In vitro (which means "in glass") fertilization (IVF) is often used for women with blocked or malfunctioning fallopian tubes , severe endometriosis , or unexplained infertility. Prior to IVF, a woman is given synthetic hormones that stimulate the maturation and release of a large number of eggs. The eggs are removed from the ovaries using an ultrasound-guided needle and combined with sperm in a laboratory dish. To increase the chances of pregnancy, four to six embryos are typically implanted into the woman's uterus when they are about three days old. Extra embryos may be frozen for later use.
Since multiple embryos are implanted, there is an increased chance of multiple births and the associated risks to both mother and children. "Selective reduction," or abortion of one or more fetuses, may be used to reduce the number of multiples. IVF is expensive ($8,000 to $10,000 per trial) and the likelihood of producing a child using IVF decreases with increased maternal age. In addition, the success rate is typically less than 20 percent, although it varies by clinic and is improving as the procedure becomes more common.
Gamete Intrafallopian Transfer. Gamete intrafallopian transfer (GIFT) is similar to IVF except that eggs and sperm are mixed and placed immediately into the woman's fallopian tubes using laparoscopic surgery . In zygote intrafallopian transfer (ZIFT), eggs and sperm are fertilized in the laboratory, but the resulting zygotes are not incubated and are placed in the woman's fallopian tubes rather than her uterus. Although more complicated, GIFT and ZIFT are thought to more closely simulate natural events and have a higher (5 to 10 percent higher) success rate than IVF. Unfortunately, women with severely diseased fallopian tubes cannot use them.
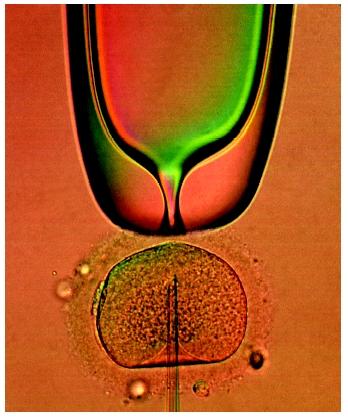
Intracytoplasmic Sperm Injection. In intracytoplasmic sperm injection (ICSI), a single sperm is injected directly into an egg using a tiny glass needle to create an embryo prior to in vitro fertilization. ICSI therapy can be used when sperm are scarce, have poor motility, or are otherwise unable to fertilize an egg. Because the procedure has only been in effect since the early 1990s, the side effects of ICSI are not well known but may include genetic or chromosomal abnormalities, major birth defects, and infertility (particularly in males).
Embryo Adoption
Embryo adoption is a procedure in which an embryo created from the egg of a woman and the sperm of a man is transferred into the uterus of another woman to be raised by her and her partner. Embryos for "pre-birth adoption" may be surplus frozen embryos from IVF donated by the genetic parents or embryos created specifically from egg and sperm donors. In both cases, the embryo has no genetic relationship to its parents.
Surrogate Mothers
A surrogate mother is a woman who signs a contract with a man to be artificially inseminated with his sperm, give birth to the child, then turn the child over to the man and his partner at birth. The man and his partner usually legally adopt the child. Alternately, embryos created through IVF can be implanted into a surrogate mother if the female partner is unable or unwilling to go through a pregnancy herself. Surrogate mothers are paid for their expenses and receive an additional fee. Agencies and/or lawyers are often involved in the process.
The use of reproductive technologies by single people, postmenopausal women, homosexual couples, and others is increasing since the technologies give people more choices about when and how to become a parent as well as some control over the genetic quality and even the sex of the offspring. However, reproductive technologies also bring with them complex social, psychological, and ethical considerations, and the multi-billion-dollar industry has little regulation. Egg, sperm, and embryo donors may worry about anonymity or being sued for child support. Children may want the right to know their medical history and perhaps their biological parents and siblings. Genetic or surrogate parents may want to claim the children they have helped produce. Couples may argue about custody of frozen embryos or disposal of extra or inferior embryos. Others may question the ethics of selling eggs, sperm, and "womb space."
SEE ALSO Birth Control ; Chromosome Aberrations ; Clone ; Female Reproductive System ; Sexual Reproduction
Lynnette Danzl-Tauer
Bibliography
Bach, Julie S., ed. "Should Limits Be Placed on Reproductive Technology?" In Biomedical Ethics: Opposing Viewpoints. San Francisco, CA: Greenhaven Press, 1998.
Lasker, Judith N., and Susan Borg. In Search of Parenthood. Philadelphia, PA: Temple University Press, 1994.
Nordenberg, Tamara. "Overcoming Infertility." FDA Consumer 31, no. 1 (1997): 18.
Sesson, Donna R., Diane G. Hammit, Mark A. Domario, and Daniel A. Dumesic. "Recent Advances in Infertility Treatment." Minnesota Medicine 81 (1998): 27–32.
Wright, Karen. "Human in the Age of Mechanical Reproduction." Discover 19, no. 5 (1998): 74–81.
Comment about this article, ask questions, or add new information about this topic: