Bone
Bone serves many important functions. Bones support the body, protect underlying organs, and provide a movable skeleton against which the muscles can work. In addition, bone forms all the cells of the blood, plus takes part in calcium and acid-base balance, and storage of trace elements (such as zinc) needed by cells elsewhere.
Bone Structure
Bone is created from osseous connective tissue . Like other types of connective tissue, osseous tissue is composed of relatively sparse cells surrounded by an extracellular network, or matrix . Bone matrix is a tough, resilient mixture of protein and minerals . Osteoblasts, a type of bone cell, secrete proteins into the matrix, which provide tensile strength (resistance to stretching and twisting). The principal protein of the bone matrix is collagen, which accounts for almost one-third of the dry weight of bone. Most of the rest of the bone's weight is due to the minerals of the matrix. These are mainly calcium phosphate and calcium carbonate. Embedded in the protein network, the minerals provide hardness and compressive strength.
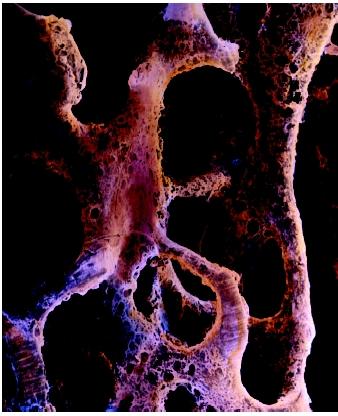
Bone cells remain alive and, like other cells in the body, must be nourished by blood. In order to deliver nutrients to and remove waste from the bone interior, the hard, compact surface is pierced by "canals" through which blood vessels can travel. Once inside, these canals branch, allowing blood vessels to reach cells throughout the bone. This canal system gives bone its characteristic appearance under the microscope, with bone cells embedded in concentric rings (lamellae) of calcified matrix, all surrounding a hollow canal. These units of structure, called osteons, all run parallel in compact bone, but form a looser and less-ordered network in spongy bone. Compact bone forms in the perimeter of long bone shafts, such as those of the legs and arms, where stress forces tend to be all in the same direction. In contrast, spongy bone is found in the ends of bones, where forces come from many different directions. Spongy bone also occurs where bone is not subject to significant stress.
Formation and Growth
Ossification (bone formation) occurs in one of two ways. Intramembranous ossification occurs within parts of the skull and part of the clavicles . In this process, osteoblasts deposit matrix on a membranous network within the
By contrast, most of the body's bones form by endochondral (within cartilage) ossification. In this process, a temporary model in the shape of the future bone is made from cartilage laid down by chondrocytes (cartilageforming cells), which later die within the shaft of the future bone. The space created by the death of these cells is invaded by osteogenic (bone-forming) cells. These cells differentiate into osteoblasts and secrete the matrix. As osteoblasts build bone, another type of cell, the osteoclast, dissolves older matrix, enlarging the cavity within. Osteoclasts dissolve matrix by secreting hydrochloric acid, which attacks the mineral portion, and enzymes that digest the collagen and other proteins. Within the shafts of the long bones, the spaces created are filled with blood-forming tissue, the bone marrow.
Hormonal Control
Growth in bone length is stimulated by sex hormones and growth hormone during puberty, accounting for the pubertal growth spurt. Growth is later halted, and bones cannot grow in length during adulthood. However, bone is constantly remodeled by the combined action of osteoblasts and osteoclasts, and can grow in width in response to mechanical stresses such as weight lifting. When a bone is fractured, chondrocytes, osteoblasts, and osteoclasts go to work repairing it and cleaning up the damage.
The interactions of three hormones—parathyroid hormone, calcitonin, and calcitriol—control bone growth and remodeling, as well as the calcium concentration in the blood serum. Calcium is necessary for a variety of critical functions outside of bone, including muscle contraction, neuron function, glandular secretion , and blood clotting. Because of this, serum calcium is kept within very narrow limits, 9.2 to 10.4 milligrams per deciliter of blood. Calcium excesses and deficiencies are prevented by using bone as a storage pool.
Calcitriol promotes calcium absorption from the gut and prevents its loss through the kidneys. Calcitriol is made from vitamin D, either supplied from the diet or manufactured by skin cells exposed to sunlight. A lack of vitamin D can lead to rickets in childhood, osteomalacia in adulthood, or osteoporosis later in life. Once calcium is absorbed by the gut, it enters the blood, and, if in high concentration, is deposited in bone by osteoblasts, stimulated by calcitonin. When serum calcium levels drop, parathyroid hormone indirectly causes osteoclasts to break down bone and release calcium into the blood. Bone, therefore, is constantly cycling between deposition and resorption, and about one-fifth of the skeleton is built and demolished each year.
SEE ALSO Blood ; Connective Tissue ; Musculoskeletal System ; Vitamins and Coenzymes
Angie Kay Huxley
Bibliography
Alexander, R. M. Bones: The Unity of Form and Function. New York: Macmillan, 1994.
Ross, M. H., L. J. Romrell, and G. I. Kaye. Histology: A Text and Atlas, 3rd ed. Baltimore, MD: Williams & Wilkins, 1995.
Turner, C. H. "Homeostatic Control of Bone Structure: An Application of Feedback Theory." Bone 12 (1991): 203–217.
Zaleske, D. J. "Cartilage and Bone Development." Instructional Course Lectures 47 (1998): 461–468.
Some forms of osteoporosis (brittle bones) are caused by overactive osteoclasts.
Mind expanding!